Complications from Brachioplasty (Arm lift) Surgery: What Patients Need to Know
Brachioplasty, often described as arm lift surgery or brachioplasty arm lift surgery, is a surgical procedure performed to reduce excess skin and, in selected cases, excess fat from the upper arms. It is commonly undertaken after significant weight loss, including after bariatric surgery, or when reduced skin elasticity results in persistent loose skin that does not resolve with exercise.
As with any surgical procedure, brachioplasty surgery carries risks. While many patients progress through the recovery process without major issues, complications can and do occur. Understanding the nature of these risks, how often they occur, and how they are managed is essential to informed decision-making.
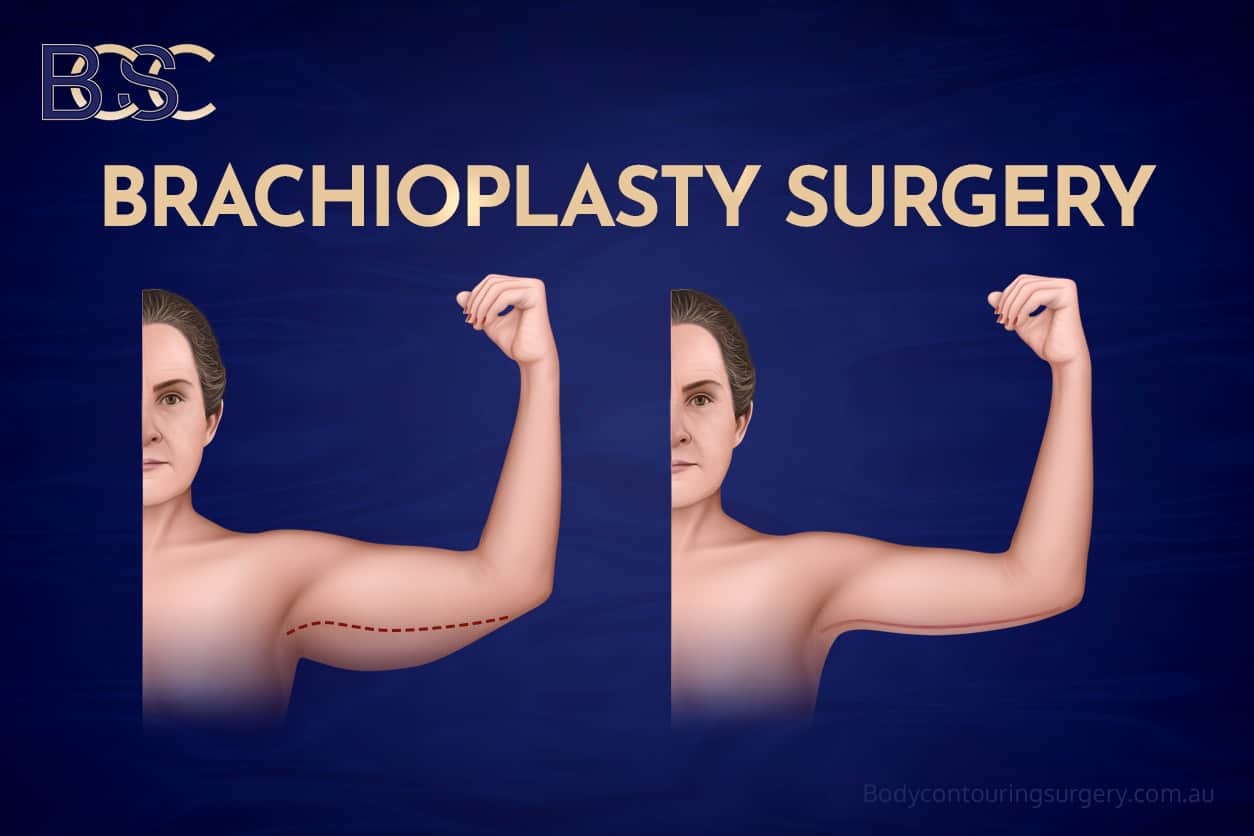
This article outlines the known complications from brachioplasty, drawing on published research to provide realistic complication rates, clear explanations, and practical context. It is written to support patients considering an arm lift (brachioplasty) in developing realistic expectations about the healing process and potential surgical outcomes.
How Common Are Complications After Arm Lift (brachioplasty) Surgery?
Brachioplasty (arm lift) surgery is associated with a higher overall complication rate than many shorter or less extensive procedures. This is largely due to the length of the incision, the degree of tension at the incision site, and disruption of underlying tissues, such as lymphatic channels and sensory nerves.
Across multiple studies, reported overall complication rates range from 20–40%, with the majority categorised as minor complications that resolve with appropriate management [1–3]. Patients who have experienced significant weight loss have a higher risk of complications compared with those undergoing arm lift surgery for mild skin laxity alone [1,2].
Importantly, major complications such as blood clots, deep vein thrombosis, lung complications, or the need for blood transfusion are uncommon, occurring in fewer than 1% of cases when appropriate preventive measures are in place.
Early Complications After Brachioplasty Surgery
Bleeding and Haematoma
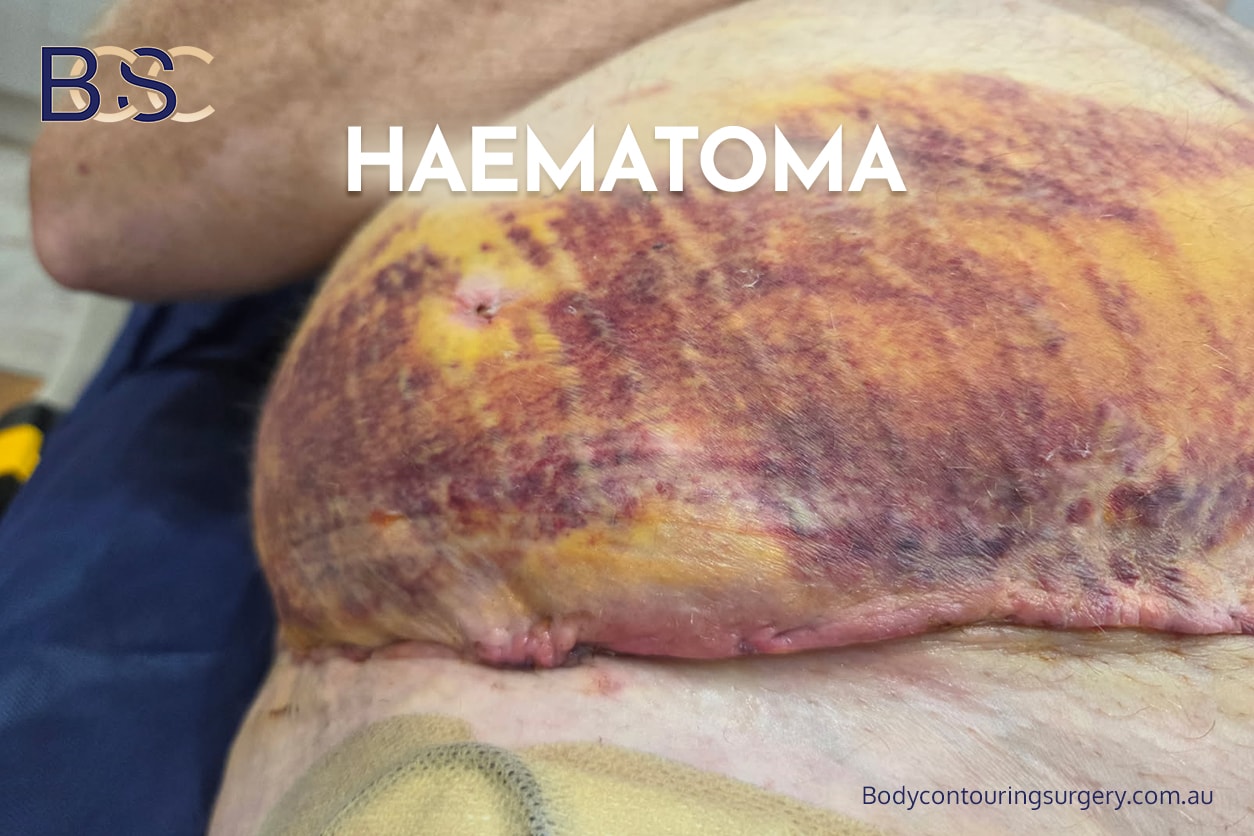
Haematoma
Incidence: approximately 1–5% [1,4]
Bleeding may occur shortly after arm lift (brachioplasty) surgery, occasionally resulting in a haematoma. A haematoma is a collection of blood beneath the skin that can increase pressure on surrounding tissues and interfere with wound healing.
Risk factors include elevated blood pressure, the use of blood‑thinning medications, prolonged surgical time, and excessive arm movement during the early recovery period. Small haematomas may be monitored, whereas larger collections usually require surgical drainage to protect the incision site and reduce the risk of infection.
Infection
Infection
Incidence: approximately 2–4% [1,3,5]
Infection following brachioplasty surgery is uncommon but important to recognise early. Most infections are superficial and occur within the first two weeks of the recovery period.
Symptoms may include increasing redness, warmth, discharge from the incision site, fever, or worsening pain. Management typically involves antibiotics and focused wound care. More severe infections may require hospital admission or further medical intervention.
Wound Dehiscence, Poor Wound Healing, and Delayed Healing
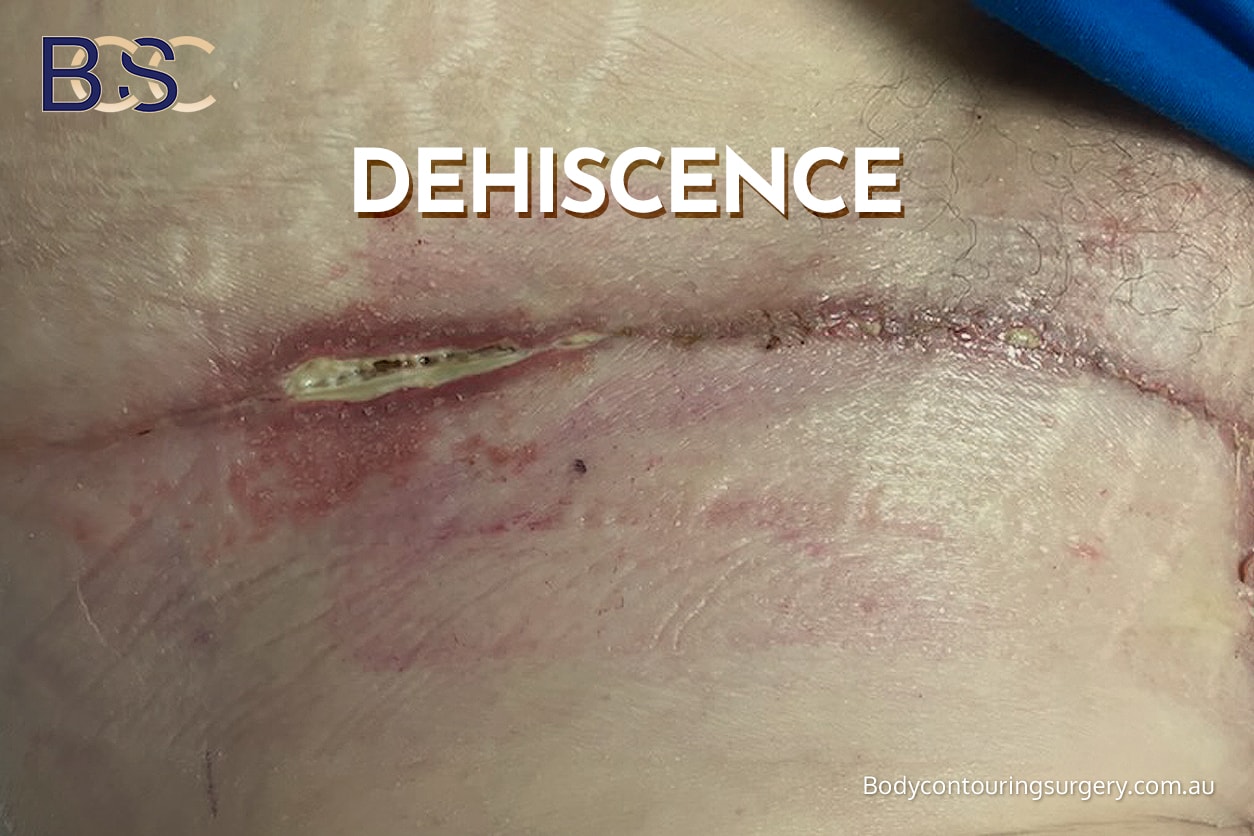
Wound breakdown (wound dehiscence)
Incidence: approximately 10–25%, higher after significant weight loss [1,2]
Delayed healing and wound dehiscence are among the most frequent complications related to arm lift (brachioplasty) surgery. These issues are particularly common near the axilla, where moisture, movement, and tension are greatest.
Poor wound healing may present as slow closure of the incision, scabbing, or small areas of separation. In most cases, these problems resolve with dressings, reduced activity, and time, without the need for revision surgery.
Seroma and Fluid Accumulation
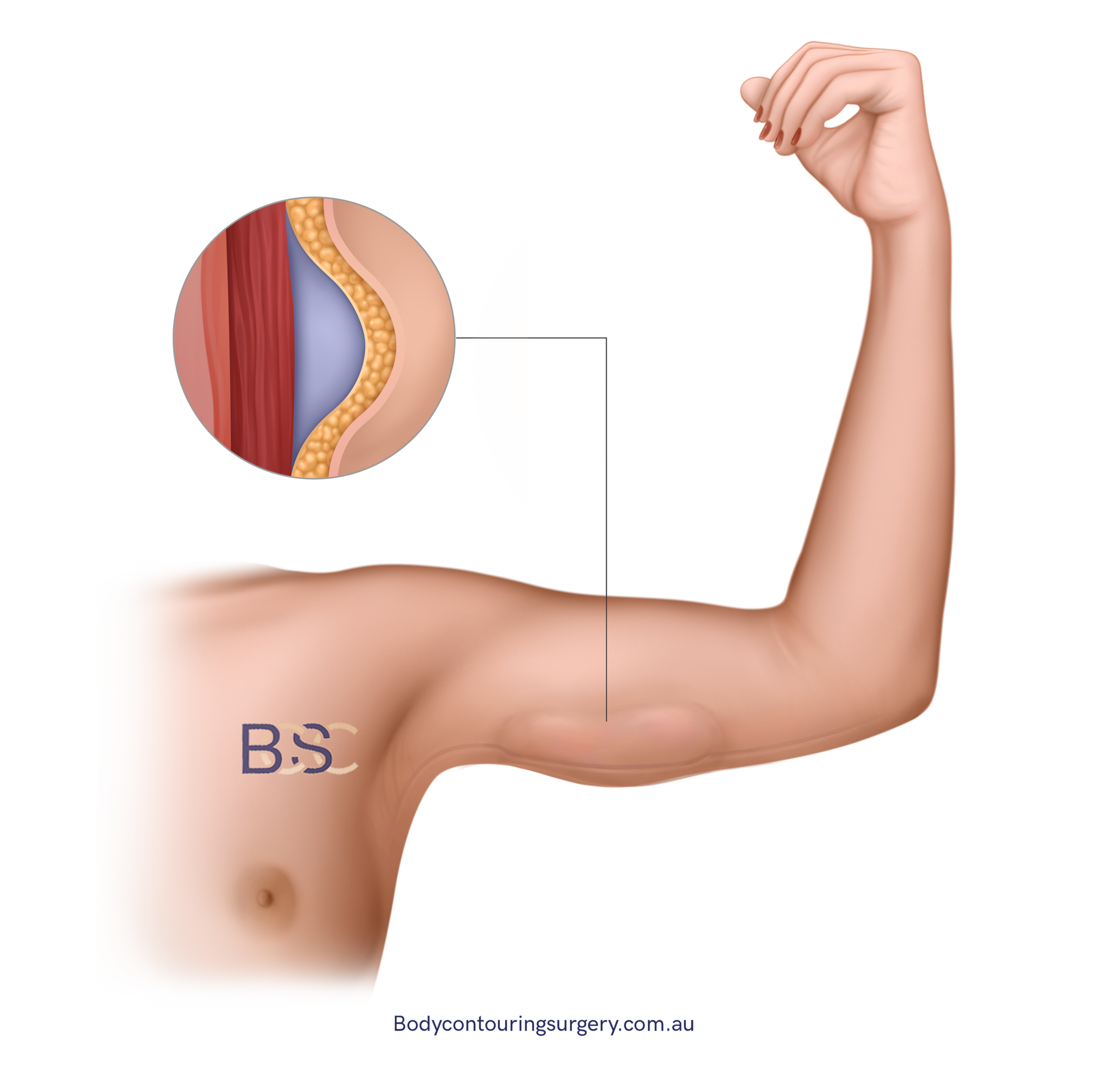
Seroma
Incidence: approximately 5–15% [1,3,6]
Seroma formation refers to fluid accumulation beneath the skin after brachioplasty (arm lift) surgery. This occurs due to the disruption of lymphatic channels and the presence of a space created by the removal of excess skin and fat.
Patients may notice swelling, asymmetry, or a fluid‑like sensation in the upper arms. Management often involves drainage procedures performed in the clinic and the continued use of compression garments. Persistent seromas may require repeated drainage or additional medical intervention.
Sensory and Nerve‑Related Complications
Nerve‑related complications
Temporary Changes in Skin Sensation
Incidence: reported in up to 70% of patients early after surgery [2,4]
Temporary numbness, tingling, or altered skin sensation is common following arm lift (brachioplasty) surgery. These changes result from stretching or interruption of small sensory nerves during brachioplasty.
For most patients, sensation gradually resolves over the healing process, although recovery can take six to twelve months.
Persistent Sensory Loss and Nerve Damage
Incidence: approximately 5–10% [1,2]
Permanent nerve damage is less common but recognised. The medial antebrachial cutaneous nerve, which supplies sensation to the inner arm, is the nerve most frequently involved.
Persistent numbness or altered skin sensation typically does not affect strength or movement but may be noticeable. Treatment focuses on education, reassurance, and the setting of realistic expectations rather than on surgical correction.
Neuropathic Pain and Neuroma Formation
Incidence: less than 2% [2,6]
In rare cases, injured nerves may develop neuromas, resulting in localised burning or shooting pain. Management may include prescribed medications, targeted injections, or surgical treatment in selected cases.
Lymphatic Complications
Prolonged Arm Swelling
Incidence: approximately 5–10% [1,3]
Ongoing swelling beyond the expected recovery period reflects temporary lymphatic disruption. This usually resolves with time, compression garments, and arm elevation.
Lymphoedema
Incidence: less than 1% [1,6]
Chronic lymphoedema following brachioplasty surgery is rare but possible. It presents as persistent swelling and heaviness of the arm and may require long‑term management with compression therapy and specialist support.
Scarring‑Related Complications
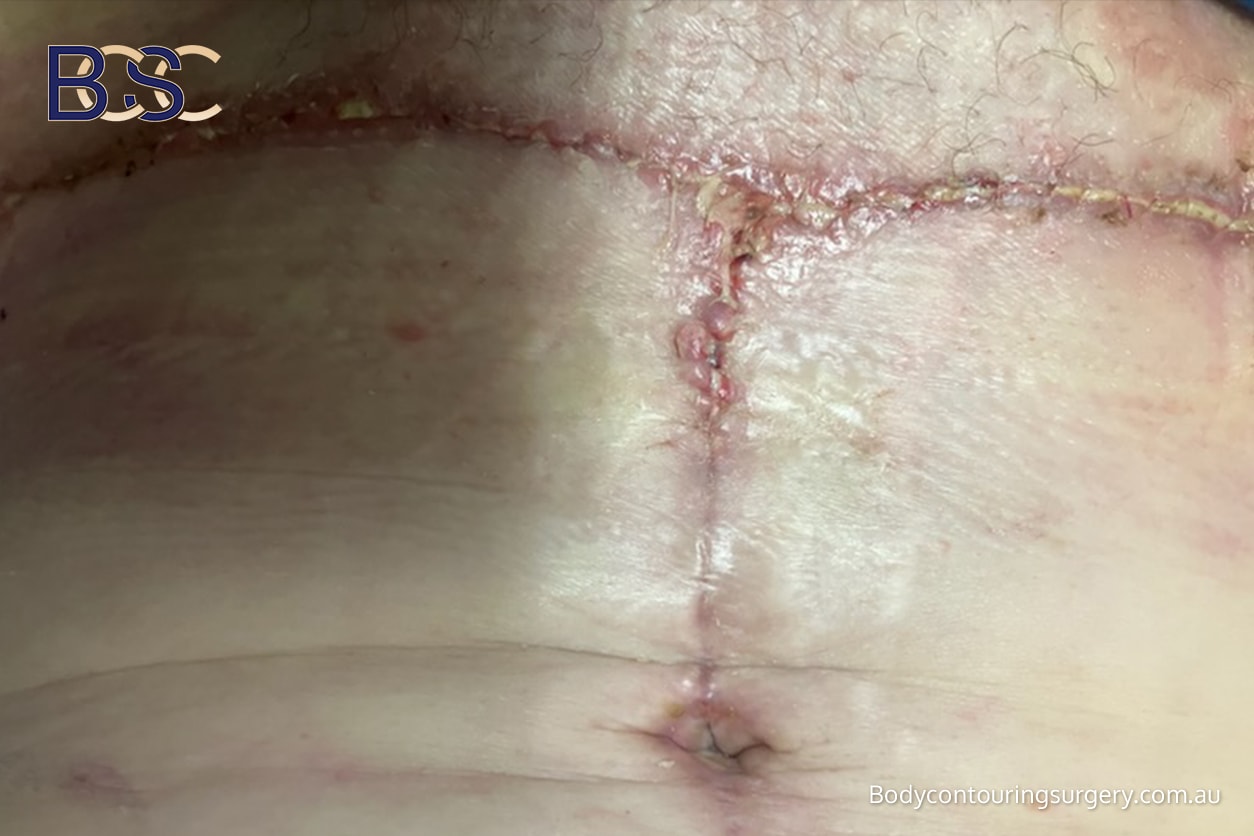
Scarring
Visible or Widened Scars
Incidence: approximately 10–30% [1,2]
Scarring is unavoidable with arm lift (brachioplasty) surgery due to the length of the incision. Some patients develop widened or more visible scars, particularly if skin elasticity is reduced or tension across the incision is high.
Scar maturation continues for 12–18 months, and appearance often resolves gradually during this time.
Hypertrophic or Keloid Scars
Incidence: hypertrophic scars 5–15%; keloid scars <5% [3,5]
Hypertrophic scars remain within the incision boundaries but may be raised or firm. Keloid scars extend beyond the incision and are more likely in genetically predisposed individuals.
Scar management strategies may include silicone therapy, steroid injections, and laser therapy where appropriate.
Aesthetic and Functional Concerns
Residual Excess Skin or Recurrent Skin Laxity
Incidence: approximately 10–20% in patients after major weight loss [1,2]
Residual loose skin may persist if skin elasticity is poor or conservative surgical techniques are used. In some cases, revision surgery may be considered once healing is complete.
Asymmetry
Incidence: approximately 5–10% [3]
Minor asymmetry between arms is common during early recovery and often resolves as swelling subsides. Persistent asymmetry may require further assessment.
Temporary Restriction of Arm Movement
Incidence: less than 5% [4]
Tight scars or protective guarding can temporarily limit shoulder or arm movement. Gradual activity progression and physiotherapy are effective treatments for this.
General Surgical Risks
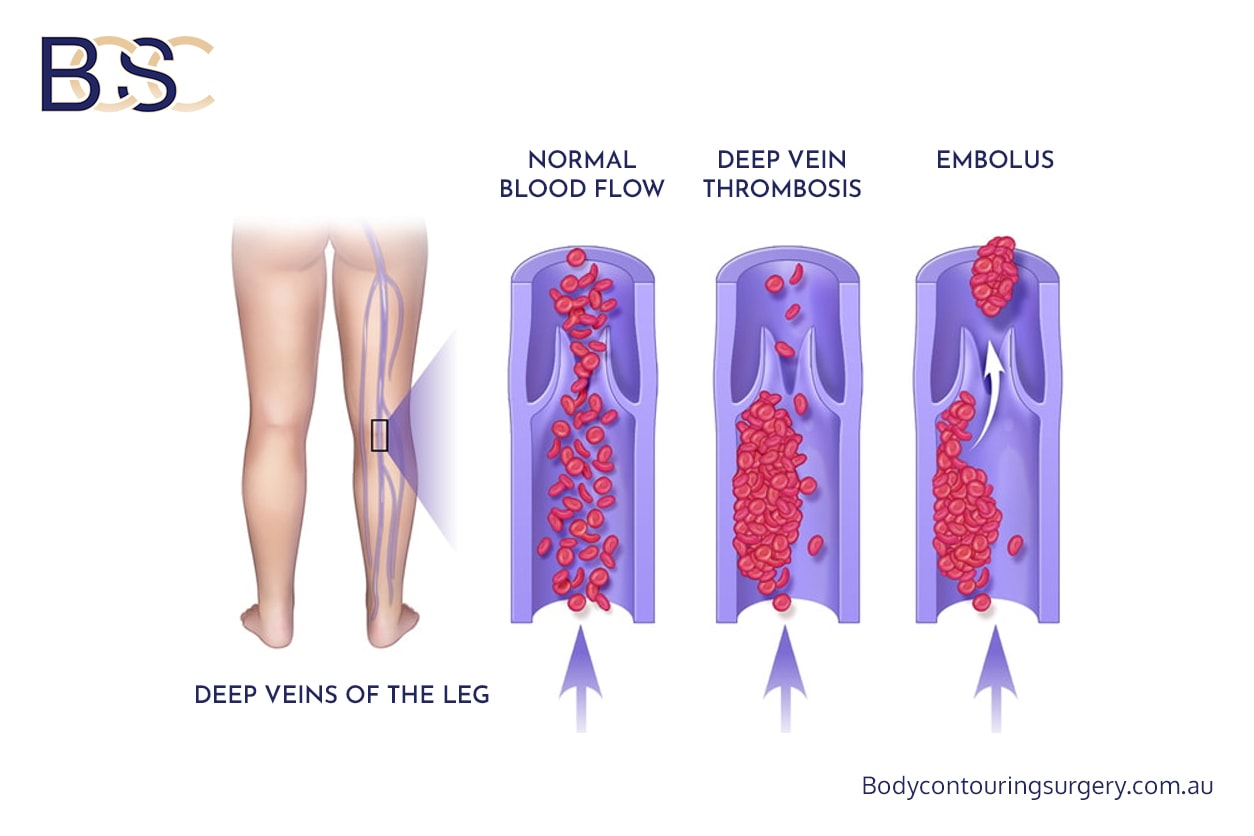
DVT
Blood Clots and Deep Vein Thrombosis
Incidence: less than 1% [4]
Blood clots, including deep vein thrombosis and pulmonary embolism, are rare after isolated arm lift (brachioplasty) surgery. Risk increases with prolonged surgery, reduced mobility, and certain medical conditions.
Revision Surgery
Incidence: approximately 5–15% [1,2]
Revision surgery may be required to treat complications such as persistent fluid accumulation, poor scarring, residual excess skin, or asymmetry. Revision procedures are generally delayed by at least 6 to 12 months after the initial surgery.
Reducing the Risk of Complications

Risk of complications
Several preventive measures can help reduce complications related to brachioplasty arm lift surgery:
- Providing a complete medical history during consultation
- Achieving and maintaining a stable weight before surgery
- Adopting a healthy lifestyle, including a balanced diet
- Avoiding smoking and nicotine, which can impede healing
- Carefully following postoperative care instructions
- Wearing and continuing to wear compression garments as advised
- Avoiding strenuous exercise and heavy lifting during the early recovery period
- Attending all scheduled follow-up appointments
These steps support wound healing, reduce fluid accumulation, and optimise overall recovery.
Frequently Asked Questions

Consultation
What is the most common complication of brachioplasty?
The most common complications from brachioplasty are delayed healing and minor wound problems, particularly near the axilla. These occur in up to 25% of patients and usually resolve with conservative management.
How risky is arm lift (brachioplasty) surgery?
Arm lift (brachioplasty) surgery does carry risks, but serious complications are uncommon. Most issues are minor and temporary, with major complications occurring in fewer than 1% of patients when appropriate precautions are taken.
What is the most common nerve injury in brachioplasty?
The most frequently affected nerve is the medial antebrachial cutaneous nerve, which can result in altered skin sensation along the inner arm.
When should unusual symptoms be reviewed?
Unusual symptoms such as severe pain, rapidly increasing swelling, fever, redness, or discharge from the incision site should prompt early review, as timely medical intervention change outcomes.
Final Considerations

Brachioplasty (arm lift) surgery can be an effective option for reducing excess skin of the upper arms, particularly after significant weight loss. However, it is not without risk. Understanding potential complications, their frequency, and how they are managed allows patients to make informed decisions and approach surgery with realistic expectations.
This information is general in nature and does not replace consultation with a qualified specialist surgeon. Outcomes vary, and all surgical procedures carry risks.
- Aly AS, Soliman S, Cram AE, et al. Brachioplasty in the massive weight loss patient. Clin Plast Surg. 2008;35(1):141‑147.
- Hurwitz DJ, Holland SW. The L brachioplasty: an innovative approach to excess tissue of the upper arm, axilla and lateral chest. Plast Reconstr Surg. 2006;117(2):403‑411.
- Hurwitz DJ. Brachioplasty. Clin Plast Surg. 2014;41(4):745‑751.
- Shermak MA, Chang D, Magnuson TH, et al. An outcomes analysis of patients undergoing body contouring surgery after massive weight loss. Plast Reconstr Surg. 2006;118(4):1026‑1031.
- Rubin JP, Michaels J. Correction of arm ptosis with medial bicipital scar. In: Strauch B, Herman C, eds. Encyclopedia of Body Sculpting After Massive Weight Loss. New York: Thieme; 2010.
- Aly AS. Complications of brachioplasty in the post–weight loss patient. Aesthetic Surg J. 2006;26(1):76‑84.