Complications Associated With Upper Body Lift (Upper Torsoplasty) Surgery in Men After Significant Weight Loss
Upper body lift surgery (upper torsoplasty) is a major body-contouring procedure that may be considered for men following significant or massive weight loss, including after bariatric surgery. The procedure aims to treat excess skin and residual tissue that may remain despite stable weight, exercise, and nutritional optimisation.
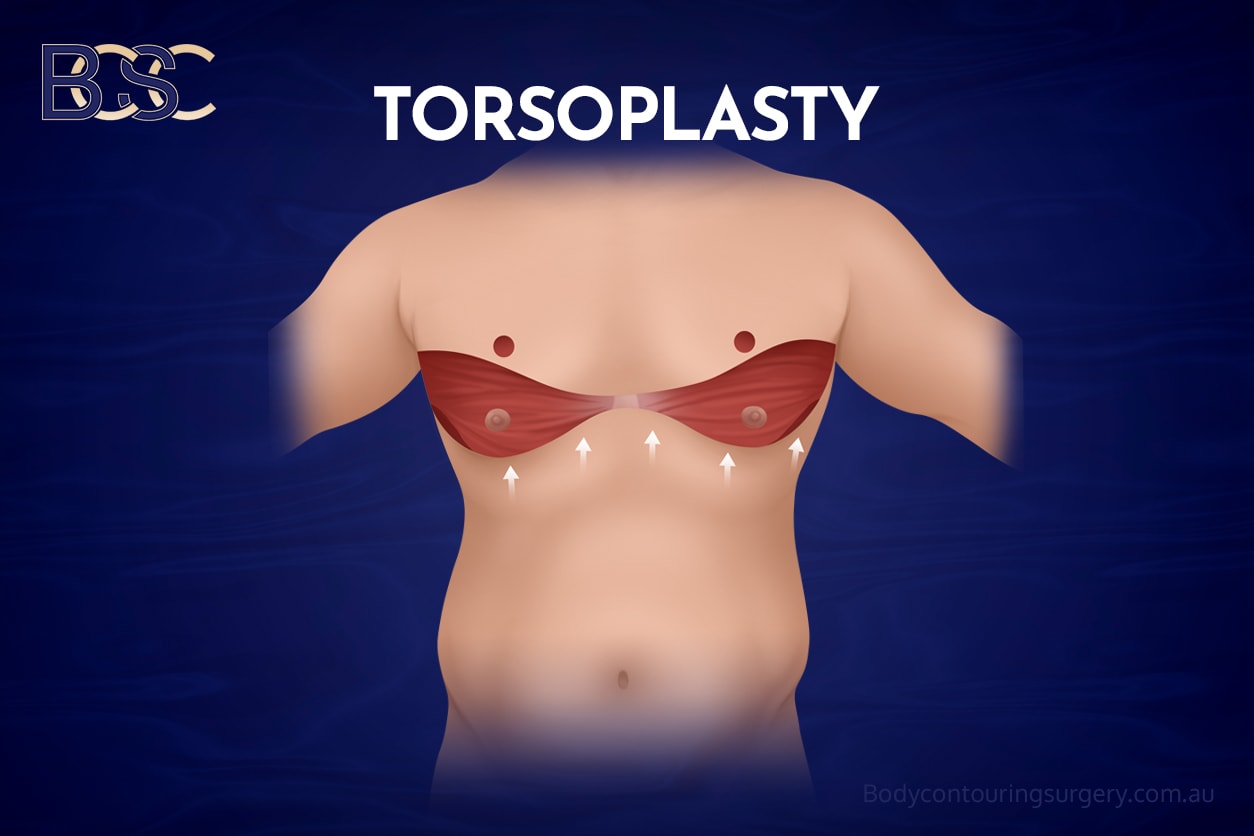
Men who have experienced substantial weight loss often present with loose skin affecting the anterior chest, lateral chest wall, axillary region, and upper back.
This article outlines the types of complications that can occur after upper body lift surgery (upper torsoplasty), why these risks exist following body lift surgery after massive or significant weight loss, and how complications are monitored and managed within a structured surgical and follow-up framework.
Overview of Upper Torsoplasty (Upper Body Lift Surgery) in Male Patients
Upper torsoplasty, also referred to as an upper body lift procedure, refers to the surgical removal of excess skin and excess fat across the upper body following post-weight-loss or massive weight loss. This type of body lift (torsoplasty) surgery may include the following:
- Anterior chest
- Lateral chest wall and axillary region
- Upper back and flank transition zones
Depending on the distribution of skin redundancy, surgery may involve:
- Anterior upper torsoplasty (chest-focused excision)
- Circumferential upper torsoplasty (chest, lateral chest, and upper back)
- VASER-assisted upper body lift (torsoplasty), where ultrasound-assisted liposuction may be used selectively to assist fat removal in conjunction with skin excision
These upper-body lift (torsoplasty) procedures are performed under general anaesthesia and typically involve long incision lines that may extend across multiple upper-body regions. As with other body-contouring procedures, including arm lift (brachioplasty), breast lift (Mastopexy), tummy tuck (Abdominoplasty), lower body lift (belt lipectomy), and thigh lift (thighplasty), incision length and tissue quality influence the risk of complications. The extent of excision, incision length, and quality of post–weight-loss skin all influence the overall risk profile.
Why Complications Are More Common After Upper Torsoplasty (upper body lift)
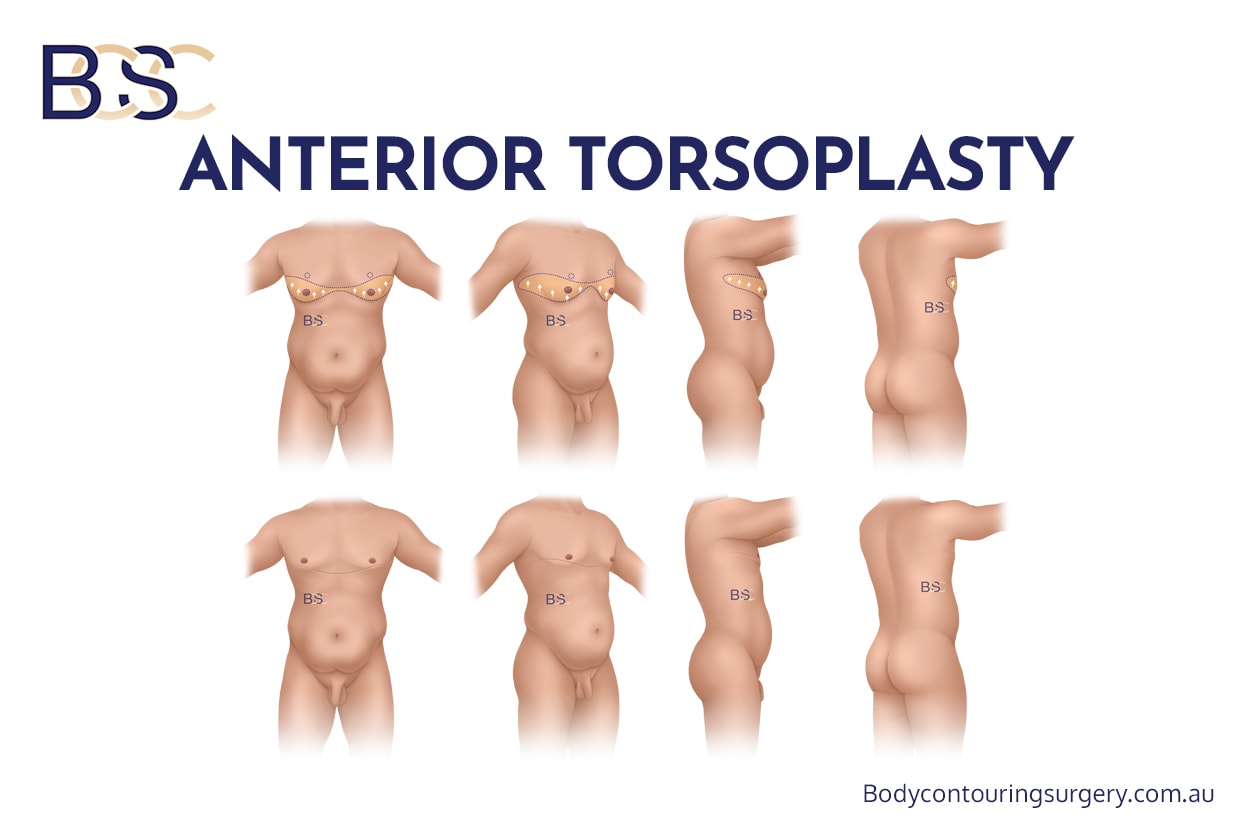
Anterior torsoplasty (Mastectomy for gynaecomastia)
Men presenting for upper torsoplasty following major weight loss often share factors that affect healing capacity.
Complication risk is increased due to:
- Reduced skin elasticity and altered blood supply following weight loss
- Large areas of skin excision create higher-tension wound closures
- Incisions crossing mobile areas such as the shoulder girdle and axilla
- Disruption of lymphatic drainage pathways in the chest wall and upper back
- Residual nutritional deficiencies, particularly after bariatric surgery
- Additional risk factors such as smoking, diabetes, or higher historical body mass index
For these reasons, upper torsoplasty generally carries higher risks than isolated chest surgery or liposuction (suction-assisted lipectomy) alone.
Early (Short-Term) Complications After Upper Body Lift Surgery
Bleeding and Haematoma
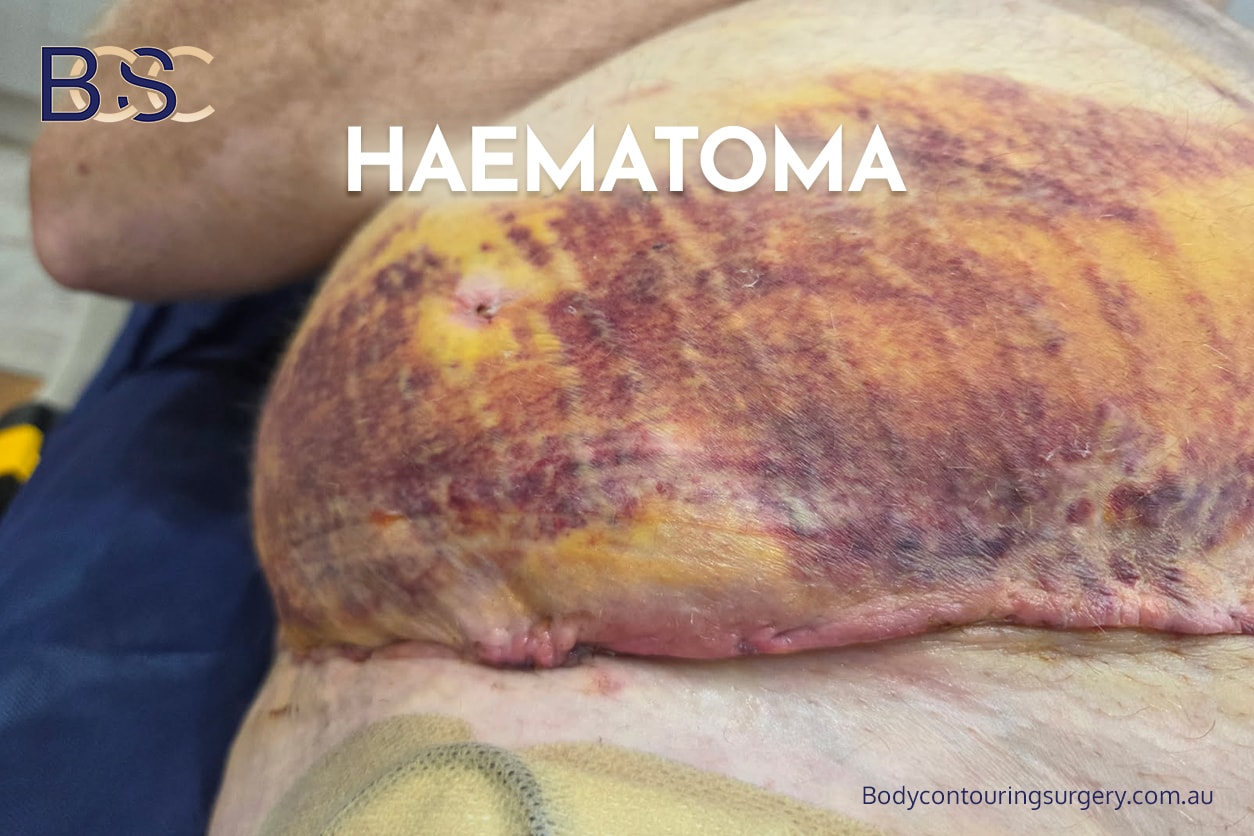
Haematoma
A haematoma is a collection of blood beneath the skin, most commonly occurring along anterior or lateral chest incisions and, less frequently, across the upper back.
Bleeding typically arises from a specific blood vessel rather than diffuse oozing. Changes in blood pressure, coughing, or early movement may contribute. Compression garments and surgical drains assist with fluid management but do not prevent active bleeding.
Small, stable haematomas may be monitored closely. Swelling, increasing pain, or skin tension requires urgent surgical assessment and may necessitate return to theatre for bleeding control.
Seroma Formation
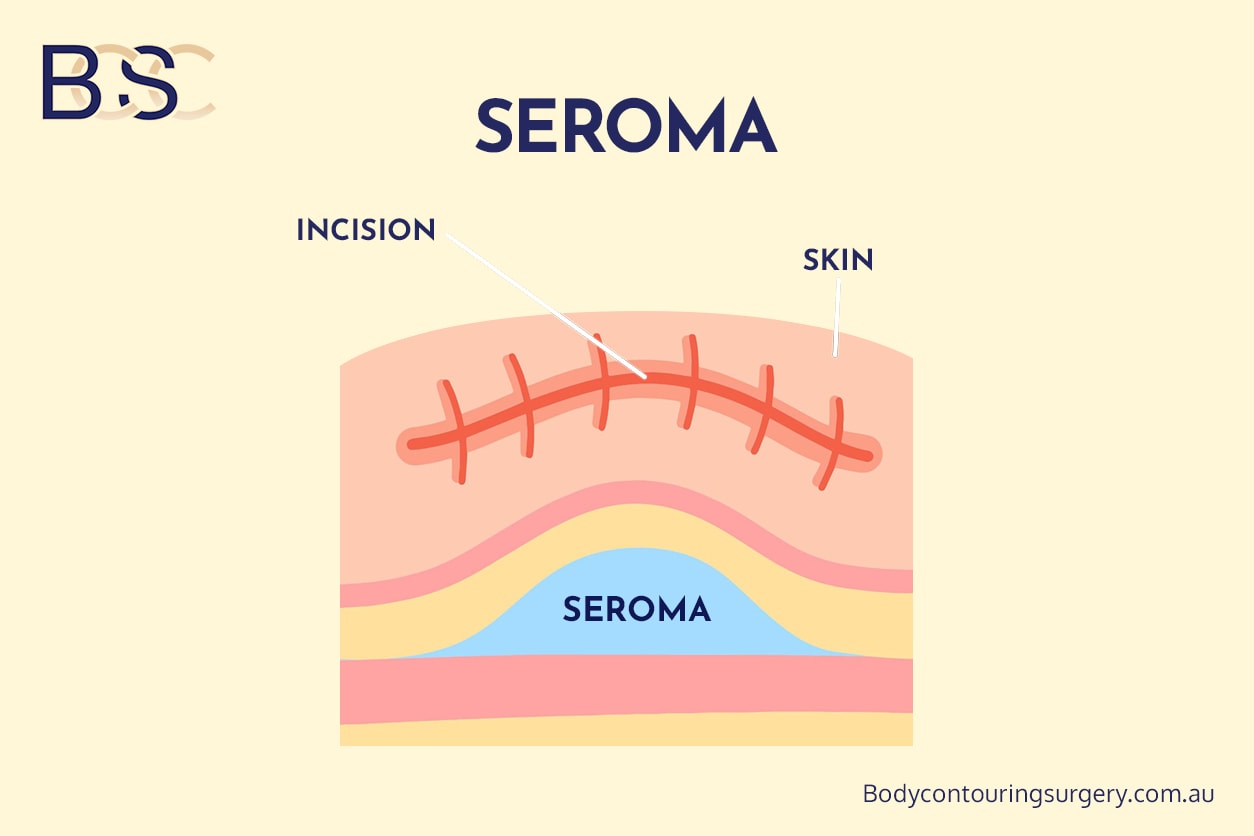
Seroma
Seromas are collections of clear fluid beneath the skin and are common following circumferential upper torsoplasty, particularly in the lateral chest and upper back.
They occur due to large tissue dissection planes and disruption of lymphatic drainage. Some seromas resolve spontaneously, while others require needle aspiration during follow-up. Repeated aspirations may be necessary. When managed appropriately, seromas rarely affect long-term contour.
Delayed Wound Healing and Wound Breakdown
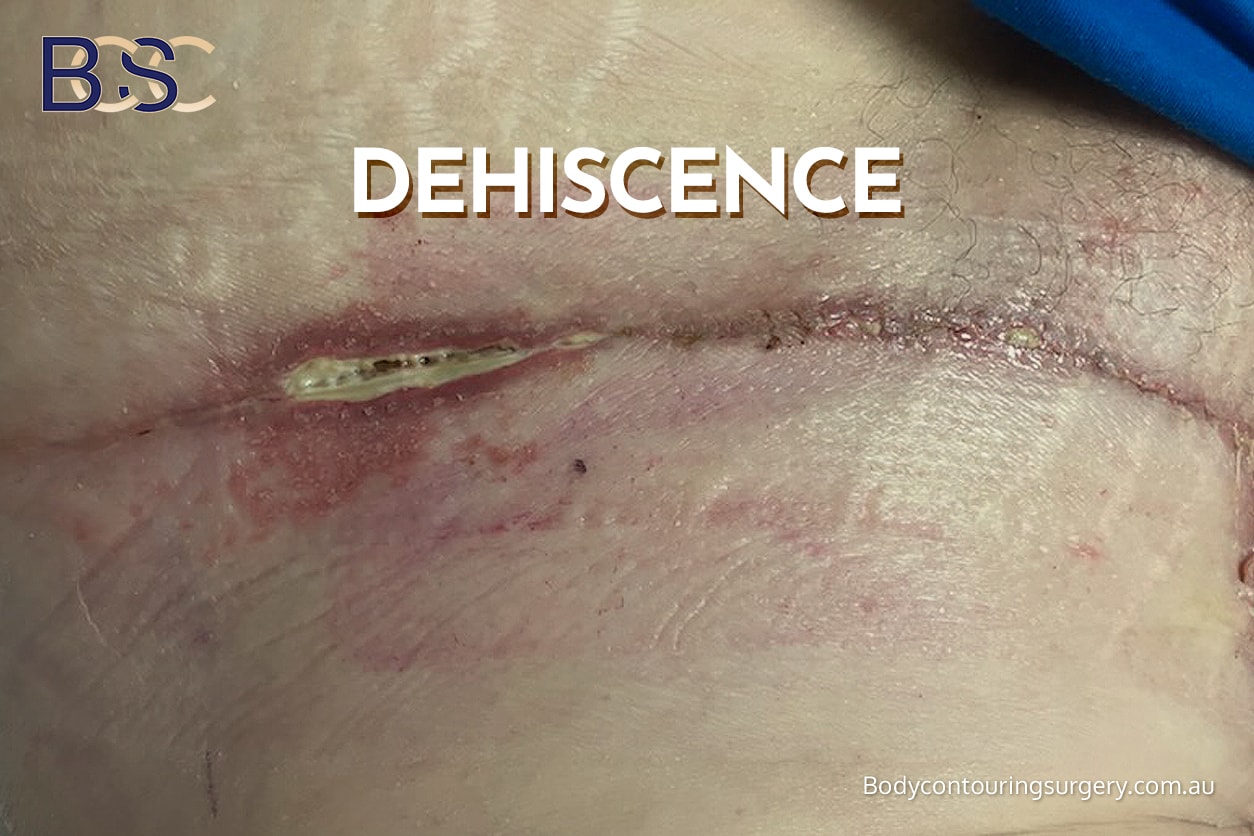
Wound breakdown (Dehiscence)
Delayed healing or partial wound separation most commonly occurs:
- Along the lateral chest wall near the axilla
- Across the upper back
- At areas of highest wound tension
Contributing factors include reduced blood supply, wound tension, infection, smoking, diabetes, or nutritional deficiency.
Small wound openings are typically managed conservatively with dressings and monitoring. Larger areas are often managed initially with wound care until healthy granulation tissue forms, after which planned surgical closure may be recommended.
Wound Infection
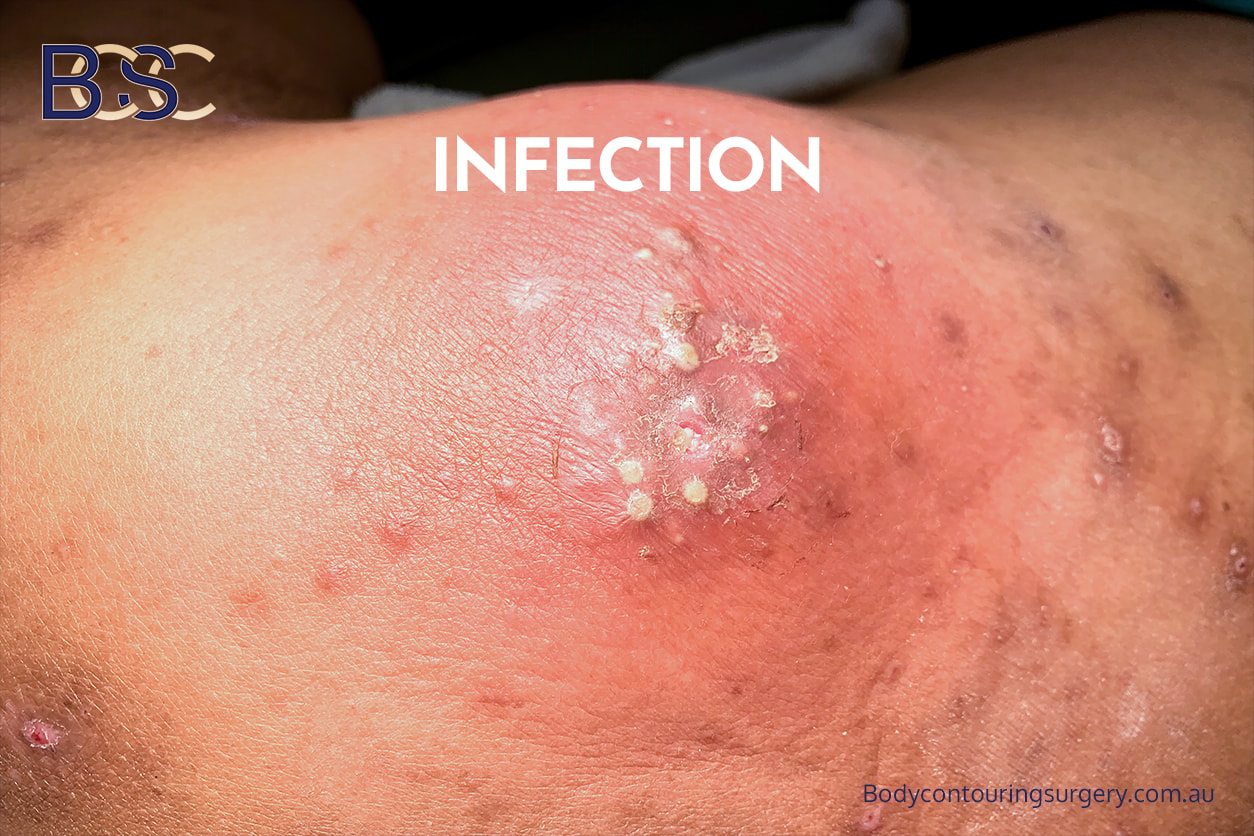
Abscess
Infection can occur along any incision line. Risk is increased by long incisions, fluid collections, and impaired healing.
Management may include antibiotics, drainage of infected collections, or surgical washout in more severe cases.
Intermediate Complications After Upper Torsoplasty Surgery
Skin or Flap Necrosis
Partial skin or flap necrosis refers to localised loss of skin along incision edges. This is more likely in high-tension areas such as the lateral chest wall or upper back.
Small areas are managed with local wound care. Larger areas may require surgical debridement and later revision, and may result in wider scars.
Nipple–Areola Complex–Related Issues
NAC (nipple areolar complex)
When the anterior chest is part of upper torsoplasty, potential issues affecting the nipple–areola complex include:
- Delayed healing
- Pigment changes
- Altered sensation
- Contour irregularity
In some cases, free nipple grafting may be used. Sensory changes and pigment alterations may resolve over time, though some changes can be permanent.
Sensory Changes
Temporary numbness or altered sensation across the chest, lateral chest wall, or upper back is common due to nerve disruption. Sensation often returns gradually over months, though some areas of altered sensation may persist long-term.
Late (Long-Term) Complications After Upper Body Lift and Body Lift Surgery
Scarring
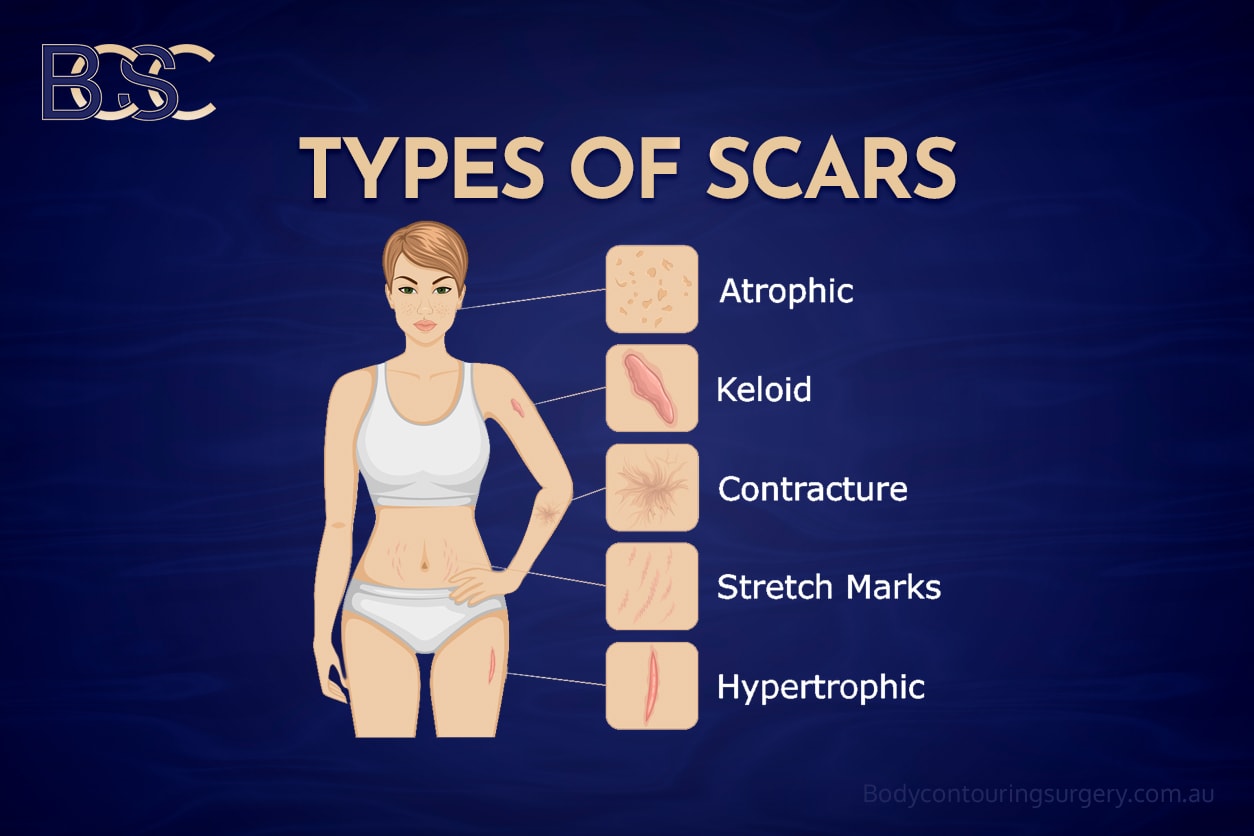
Types of scaring
Scarring is an expected outcome following upper body lift surgery. Scars may become widened, raised, thickened, or asymmetrical, particularly in high-tension areas.
Scar maturation typically takes 12–24 months. Management options may include silicone therapy, steroid injections, laser treatment, or surgical revision. Scars will soften and fade over time but remain permanent.
Residual Laxity or Contour Irregularity
Following massive weight loss, skin recoil is limited. Not all laxity can be corrected in a single procedure.
Weight stability is important. Targeted revision surgery may be considered after healing has stabilised.
Recurrent Skin Folds and Irritation
Residual skin folds may persist near the underarm, lateral chest wall, or upper back. Conservative skin care may reduce irritation. Targeted excision may be considered if symptoms are significant.
Systemic Surgical Risks
As with all major surgeries, systemic risks include:
- Blood clots, including deep vein thrombosis and pulmonary embolism
- Complications related to general anaesthesia
- Cardiopulmonary events
Rarely, internal injury may occur during liposuction-assisted procedures.
Risk reduction relies on appropriate patient selection, perioperative monitoring, early mobilisation, and structured postoperative care.
Revision Surgery

Some patients may require staged or targeted revision surgery to treat issues such as persistent seromas, scar concerns, or localised contour irregularities. Revision procedures are planned conservatively and are focused rather than extensive.
Final Considerations for Men Considering Upper Body Lift Surgery After Massive Weight Loss
Upper body lift (upper torsoplasty) surgery can provide functional and quality-of-life benefits for certain men after significant weight loss. However, it is a major reconstructive surgery with recognised risks.
Understanding the potential complications, recovery demands, and importance of structured follow-up is essential when considering upper-body lift surgery as part of post-weight-loss surgery or a broader body-contouring plan.






