Medicare and Abdominoplasty (Tummy Tuck): Understanding the Rules in Australia
Introduction: Why This Matters
For many people considering abdominoplasty, one of the first questions is: “Will Medicare cover my surgery?”
The answer is not straightforward. Medicare rebates only apply in very specific circumstances where the procedure is considered medically necessary. If the surgery is performed purely for cosmetic reasons, it will not be covered.

This guide provides a clear breakdown of:
- The Medical Benefits Schedule (MBS) item numbers that apply to abdominoplasty
- How Medicare distinguishes between cosmetic and medically necessary surgery
- What criteria you must meet after weight loss or pregnancy
- How documentation affects your claim
- Common patient questions
By the end, you’ll understand the rules that determine whether abdominoplasty (tummy tuck) is partly covered by Medicare.
Why Cosmetic Surgery Is Not Covered
Medicare’s role is to fund procedures that improve health and function. Abdominoplasty that is performed purely to change appearance is categorised as cosmetic and is not eligible for rebates.
However, if you have symptoms such as skin infections, chronic rashes, pain, or functional problems from excess skin or muscle separation (diastasis recti), abdominoplasty may be classified as reconstructive surgery.
When Abdominoplasty May Be Covered
There are two main pathways where abdominoplasty may attract a Medicare rebate.
1. After Significant Weight Loss
Medicare allows for abdominoplasty after substantial weight loss if:
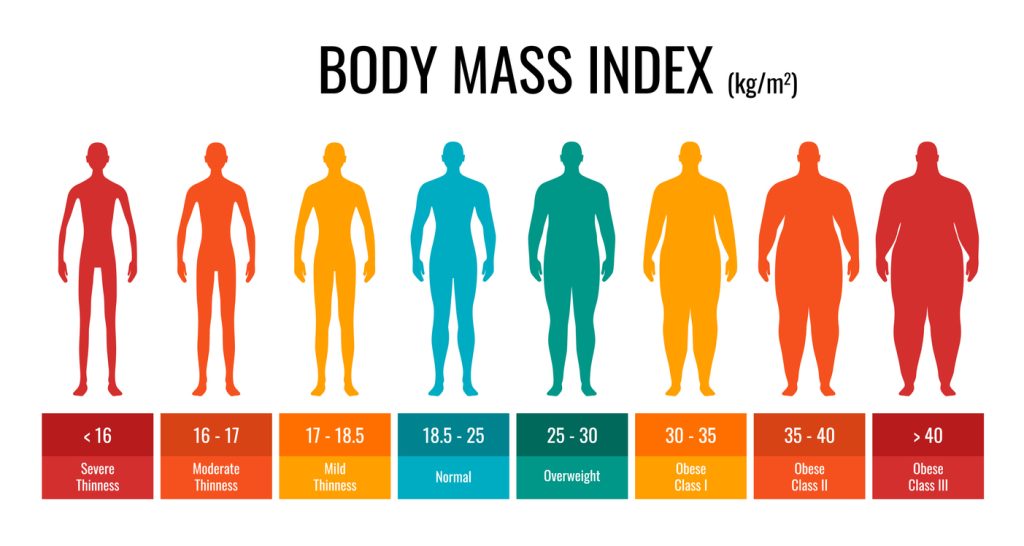
- You have lost at least 5 BMI units (Body Mass Index points)
- Your weight has been stable for at least 6 months
- You have documented functional issues such as:
- Recurrent rashes or infections under skin folds
- Pain or discomfort from overhanging skin (pannus)
- Hygiene difficulties
- Skin folds interfering with mobility or daily activity
Example: At 170 cm, a reduction of 5 BMI units equals a weight loss of approximately 14–15 kg.
2. After Pregnancy-Related Muscle Separation (Diastasis Recti)
Since July 2022, abdominoplasty may be covered for women with muscle separation (diastasis recti) after pregnancy, if:
- The muscle separation is at least 3 cm, confirmed on medical imaging
- You have symptoms such as back pain, poor core strength, or pelvic floor dysfunction
- You have completed supervised non-surgical management (such as physiotherapy) without sufficient improvement
This rule was introduced after research showed that in some women, severe diastasis recti causes persistent functional problems that conservative management alone cannot resolve.
Relevant Medicare Item Numbers
Two main item numbers apply:
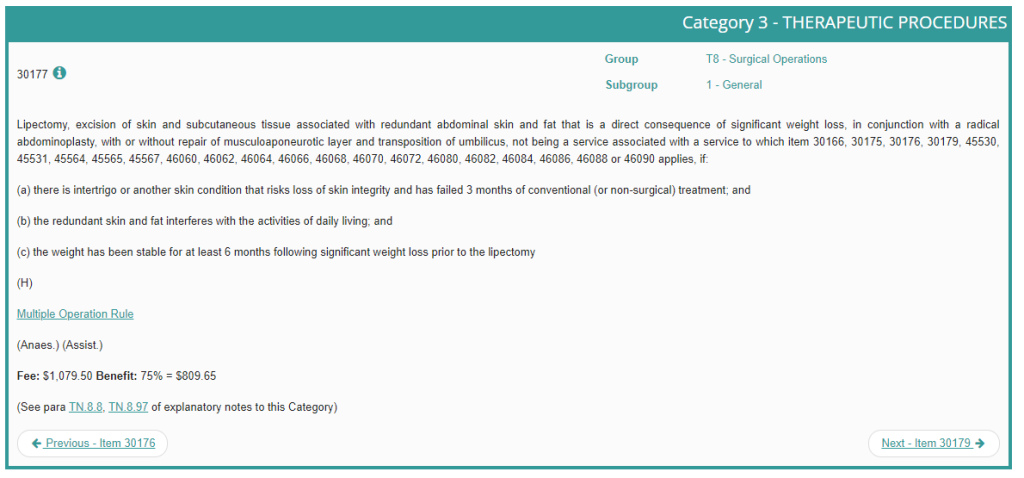
- 30177 – Abdominoplasty for patients after significant weight loss (with functional problems).
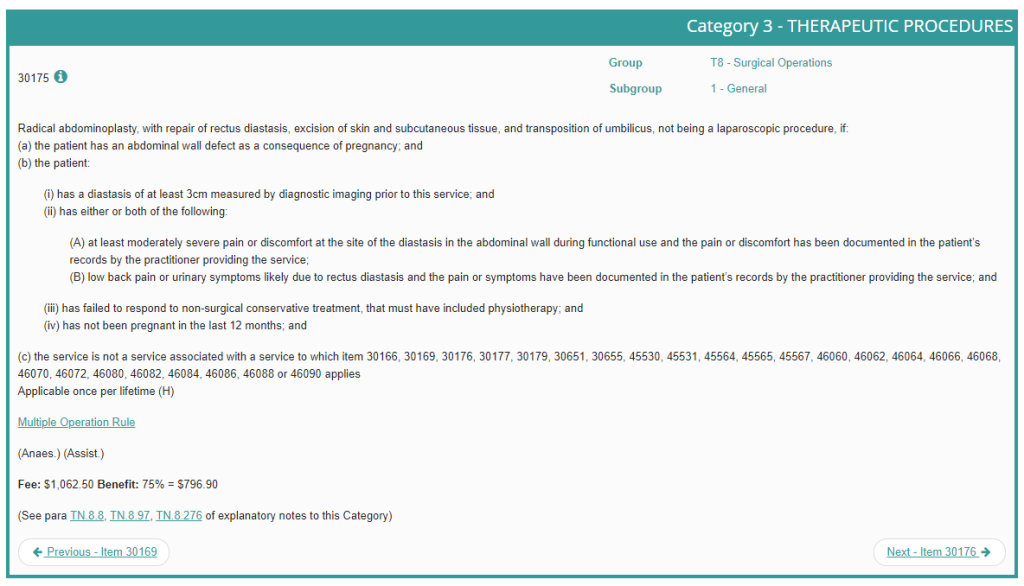
- 30175 – Abdominoplasty with repair of muscle separation (diastasis recti) after pregnancy, where symptoms persist despite physiotherapy.
Each has strict documentation requirements.
The Role of Documentation
Medicare requires:
- Medical history outlining weight loss or pregnancy changes
- Imaging or clinical measurement confirming muscle separation (diastasis recti)
- Photographs showing functional problems such as skin folds
- Notes confirming that non-surgical options have been attempted, where relevant
Without this evidence, Medicare may reject the claim.
Medicare, Private Health, and Out-of-Pocket Costs
- Medicare provides a rebate on the surgeon’s fee under the relevant item number.
- Private health insurance may contribute to hospital and theatre costs if you have the appropriate level of cover.
- Out-of-pocket costs are still common, as rebates rarely cover the full fee.
If you do not qualify under MBS rules, the procedure is classified as cosmetic and must be self-funded.
BMI Reduction Examples
FAQs
Does Medicare cover abdominoplasty after a C-section?
No, not unless there is muscle separation (diastasis recti) of at least 3 cm with ongoing symptoms and documented failed physiotherapy.
Can men qualify for a rebate?
Yes, under the weight loss criteria (30177). The pregnancy-related item number (30175) does not apply to men.
Will Medicare cover a revision abdominoplasty?
Only if functional symptoms persist and you continue to meet item number requirements. Cosmetic revision is not covered.
Can private health cover apply without Medicare?
No. Without a Medicare item number, private health funds will not contribute.
Key Takeaways
- Medicare only covers abdominoplasty when it is medically necessary.
- Eligibility criteria include weight loss with functional problems or pregnancy-related muscle separation (diastasis recti).
- Documentation and evidence are essential.
- Medicare and private health rebates may reduce costs but out-of-pocket expenses are common.
Final Word
Abdominoplasty can be life-changing for patients struggling with functional issues after weight loss or pregnancy. But the Medicare rules are strict, and not everyone will qualify.
The best way to know if you are eligible is to book a consultation with a FRACS-qualified surgeon who can assess your history, symptoms, and documentation against the MBS requirements.


