Location of practice: 30 Belmore Rd, Lorn, NSW 2320
Area of interest:
Body contouring surgery post pregnancy and post-weight loss, including Abdominoplasty, Mastopexy, Breast augmentation (Augmentation mammoplasty), Brachioplasty and Thighplasty.

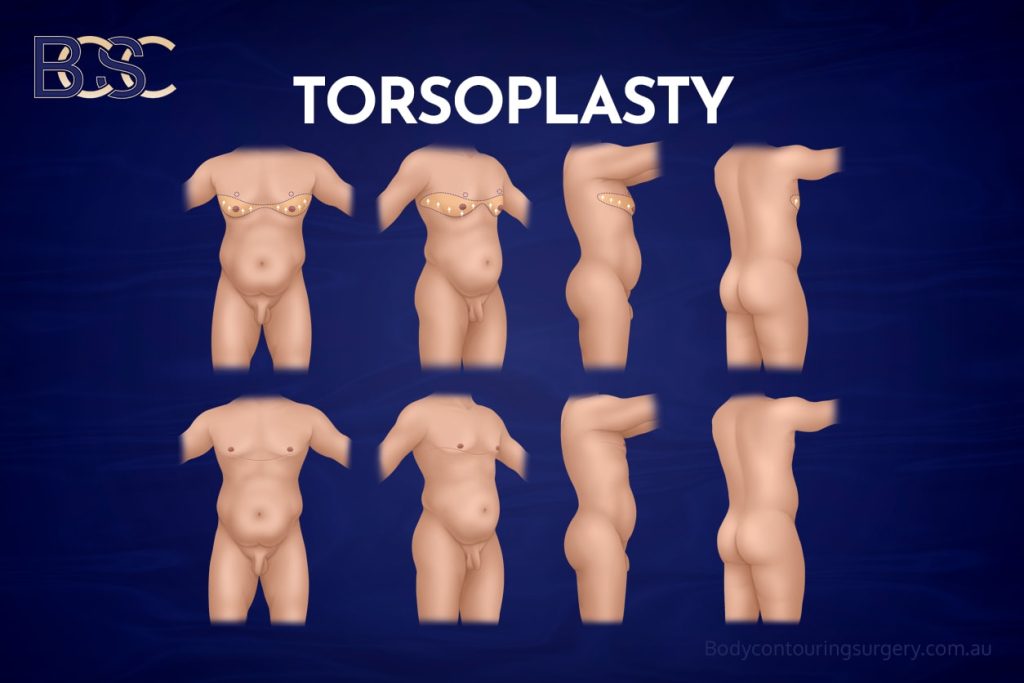
Male chest surgery after major weight loss may be considered for men who have experienced significant changes in their bodies following weight reduction and continue to have physical concerns related to excess, lax, or residual skin and fat of the chest and upper body. While weight loss is associated with benefits for metabolic health and mobility, it does not consistently reverse the structural changes in the skin and soft tissues that occur during prolonged obesity.
After massive weight loss, some men notice that the chest and upper torso retain loose or hanging tissue that does not resolve with exercise or further weight reduction. This may contribute to large skin folds, ongoing skin irritation, hygiene difficulties, and functional concerns related to clothing or physical activity. Individual experiences vary, and not all patients will experience the same degree of concern.
An upper body lift (upper torsoplasty) is a reconstructive surgical procedure that may be used to treat excess skin of the upper torso following major weight loss. At Body Contouring Surgery Clinic (BCSC), upper torsoplasty is considered part of a structured, individualised approach to post–weight-loss body contouring in men. Surgical outcomes vary between individuals.
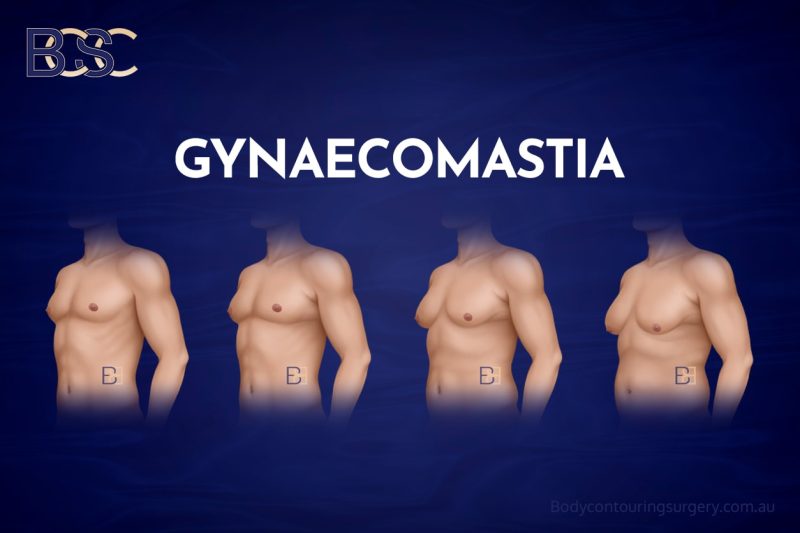
Changes in the male chest following significant weight loss are influenced by a combination of skin quality, fat distribution, and, in some patients, the presence of gynaecomastia or pseudogynaecomastia prior to weight loss.
During periods of excess body weight, the skin stretches to accommodate increased fat volume. Over time, changes in collagen and elastin can reduce the skin’s ability to retract. When weight is lost, particularly following bariatric surgery or rapid weight loss, the underlying volume decreases, but the stretched skin may not fully contract.
In addition to skin changes, breast tissue characteristics play an important role. Gynaecomastia, which involves true glandular breast tissue, is a common complaint in male patients and may coexist with weight gain. In men with significant gynaecomastia, weight loss does not reliably reduce glandular volume.
Following weight loss, these patients may be left with a fuller, more ptotic breast that retains a noticeable amount of breast tissue. In some cases, this pattern of chest change requires more extensive surgical excision to address both volume and excess skin.
By contrast, men who gain a significant amount of weight commonly develop pseudogynaecomastia, where breast enlargement is primarily related to excess fatty tissue rather than glandular tissue. This fatty enlargement stretches the skin over time.
When weight is lost, pseudogynaecomastia itself often resolves as fat volume reduces. However, the skin that was stretched during weight gain may remain lax. These patients may present with limited residual breast volume but significant loose skin.

As a result, the post–weight loss appearance of the male chest can differ substantially:
Factors that may contribute to persistent chest changes include:
As a result, some men are left with excess skin & tissue, and visible skin folds across the chest and upper body, despite reaching a stable weight.
Men presenting after massive weight loss may report concerns such as:
These concerns may be functional & physical in nature and can vary in severity between individuals.
Post–weight loss chest changes differ from standard gynaecomastia.
Management approaches differ between these conditions. Techniques used for isolated gynaecomastia may not adequately treat widespread skin laxity following significant weight loss, and treatment planning requires careful individual assessment.
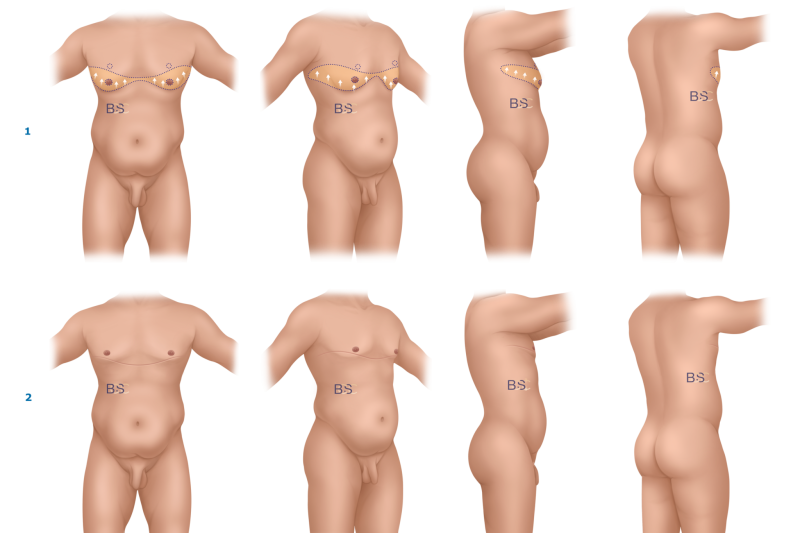
Upper body lift surgery (upper torsoplasty) is primarily indicated for men who experience significant loose skin of the upper chest and upper torso following massive weight loss. The key driver for surgery is skin excess rather than residual fat volume, and careful assessment is required to determine the pattern and extent of laxity.
In the chest, excess skin is commonly described as ptosis. In male patients, this may be defined as descent of the nipple–areola complex (NAC) below the lower border of the pectoralis major muscle, which functions as the male equivalent of the inframammary fold. In other cases, men may demonstrate pseudo-ptosis, where there is a significant amount of loose skin and residual volume within the breast envelope, even if the NAC position is relatively preserved.
Both ptosis and pseudo-ptosis can contribute to a poor chest appearance and are common indications for surgical excision following major weight loss.
The distribution of loose skin across the upper torso plays a central role in determining the appropriate surgical approach.
When excess skin is predominantly located on the anterior chest, with minimal involvement of the lateral chest wall or upper back, an anterior upper torsoplasty may be considered. This approach focuses on excision of redundant skin across the chest and upper abdomen while limiting the extent of posterior scarring.
Anterior torsoplasty is commonly indicated in patients with chest ptosis or pseudo-ptosis, where skin excess is confined to the anterior torso.
When loose skin extends beyond the anterior chest to involve the lateral chest wall and upper back, an upper circumferential torsoplasty may be indicated. In these patients, treating the chest alone may leave residual folds or contour imbalance.
Circumferential torsoplasty allows for excision of excess skin across the chest, bra line region, and upper back, providing a more balanced correction of the upper torso. Not all patients require circumferential treatment, and the decision is individualised.
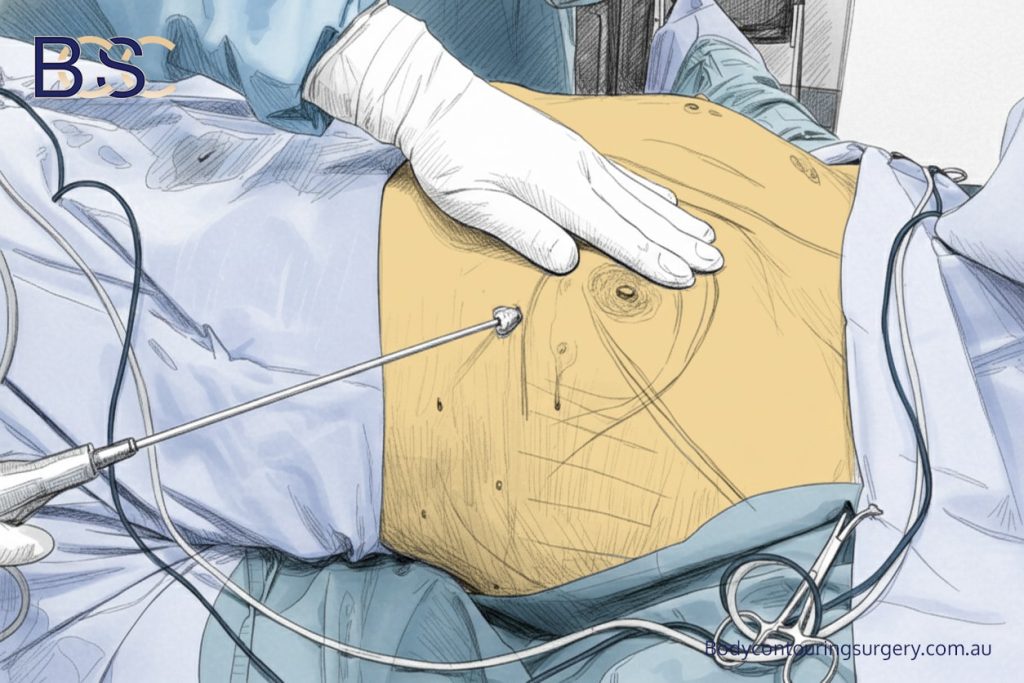
In men following massive weight loss, liposuction is not always required as part of upper torsoplasty. Many patients have already lost substantial fat volume, and the primary issue is excess skin rather than excess fat.
In selected cases, liposuction (suction-assisted lipectomy) may be added as an adjunct to treat focal areas of residual fat or to refine contour. The decision to include liposuction is based on physical examination findings and is not routine for all post–weight loss patients.
Upper torsoplasty may be considered in patients who:
A comprehensive medical history, physical examination, and discussion of alternative management options are essential components of the consultation process.
Upper body lift surgery (upper torsoplasty) is performed under general anaesthesia. The procedure involves careful dissection through tissue layers while preserving blood supply and minimising trauma to surrounding structures.
The surgical approach is planned to balance tissue removal with wound healing. Individual operative details vary.
Patients typically remain in the hospital for one to two nights, depending on the extent of surgery and individual recovery. Pain management is provided using appropriate pain medications, and early gentle mobilisation is encouraged to reduce the risk of blood clots.
Surgical drains may be used temporarily to manage fluid accumulation.
Recovery following upper torsoplasty varies between individuals and depends on the surgical extent. General timelines may include:
Patients are provided with individualised postoperative instructions. A compression garment is recommended during recovery.
Incision sites are reviewed during scheduled follow-up appointments to monitor wound healing. Once wounds have healed, silicone-based products may be considered for scar management.
Scarring is an expected outcome of surgery. Scar appearance and maturation vary between individuals and over time.
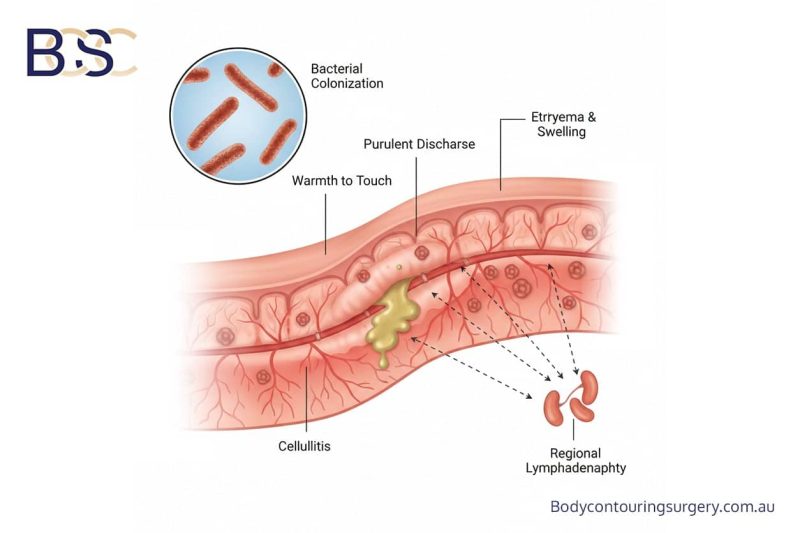
Upper torsoplasty is a major surgical procedure and carries recognised risks, which may include:
A detailed discussion of risks, potential complications, and alternative options forms part of the informed consent process.

Some patients report physical comfort or ease of daily activities following upper torsoplasty; however, outcomes vary. Long-term results depend on factors such as weight stability, healing, and individual health.
Torsoplasty refers to surgical procedures that remove excess skin and tissue from the torso (chest) following significant weight loss.
Recovery timelines vary. Initial recovery commonly spans several weeks, with ongoing changes over several months.
In cases where excess skin is present, surgical skin removal may be discussed as one management option following assessment.
Activity restrictions, including avoidance of heavy lifting and strenuous exercise, are commonly advised during early recovery. Individual guidance is provided by the treating surgeon.
An upper body lift (upper torsoplasty) is a reconstructive surgical option that may be considered for selected patients following massive weight loss. It is not suitable for everyone, and outcomes vary between individuals. This information is general in nature and does not replace consultation with a qualified medical practitioner.